Support Page Content
Traumatic Brain Injury Research Projects
Traumatic Brain Injuries: An Overview
A concussion is a type of traumatic brain injury—or TBI—caused by a bump, blow, or jolt to the head or by a hit to the body that causes the head and brain to move rapidly back and forth. This sudden movement can cause the brain to bounce around or twist in the skull, creating chemical changes in the brain and sometimes stretching and damaging brain cells. Medical providers may describe a concussion as a “mild” brain injury because concussions are usually not life-threatening. Even so, the effects of a concussion can be serious.
Source: Centers for Disease Control and Prevention (CDC). (2020, September). Traumatic Brain Injury & Concussion: Get the Facts About TBI.
What You Need To Know About Traumatic Brain Injury (Video)
TED TALK - A Brain Injury Is Like A Fingerprint, No Two Are Alike (Video)
What Happens When You Have A Concussion? (Video)
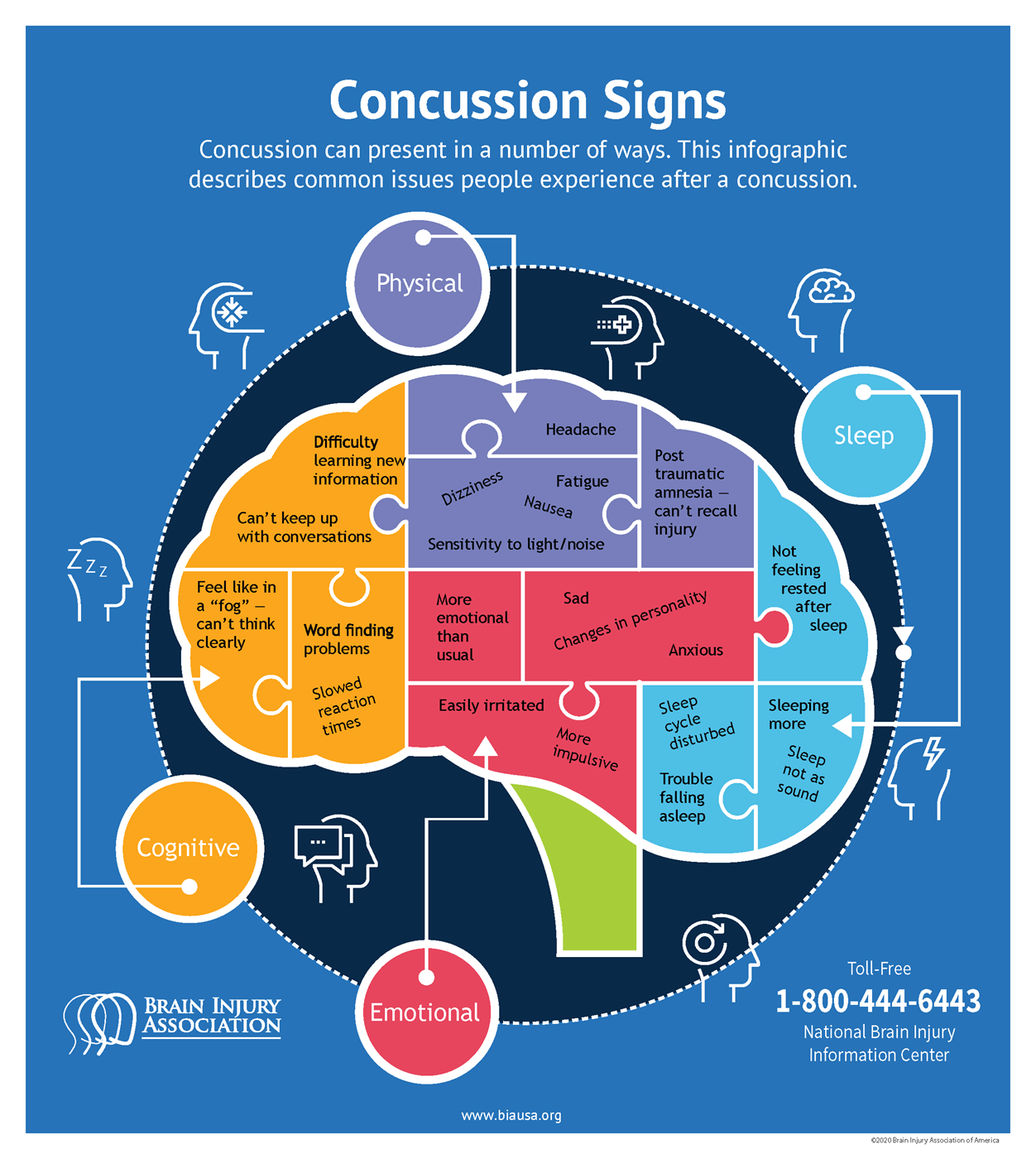
Concussion Signs & Symptoms (Video)
According to the Centers for Disease Control and Prevention (CDC), "A traumatic brain injury, or TBI, is an injury that affects how the brain works that may be caused by a bump, blow or jolt to the head. TBI is a major cause of death and disability in the United States" (CDC, 2020). There are three main types of TBI: mild TBI or concussion (mTBI), moderate TBI, and severe TBI. With over 2 million occurrences and approximately 50,000 deaths annually, TBI is the leading cause of death in young adults (<45 years of age). TBI is associated with $76.5 billion in direct and indirect medical costs (Siebold et al., 2018). Anyone can experience a TBI, but statistics suggest that particular groups are at a higher risk of obtaining a TBI or having poorer health outcomes after the injury. The CDC states that groups who are more likely to be affected by TBI include: racial and ethnic minorities, service members and veterans, people who experience homelessness, people who are in correctional and detention facilities, survivors of intimate partner violence, and people living in rural areas (CDC, 2020).
Individuals may acquire a TBI from various accidents; however, the most common TBI injuries result from falls, firearm-related injuries, motor vehicle crashes, and assaults (CDC, 2020). The effects of these injuries can lead to short-term or life-long health and cognitive-communication challenges. For example, initial and persistent cognitive-communication deficits are the most common complaints after TBI and the biggest challenge to independent living, social re-adaptation, engagement in family life, and participation in everyday activities (McAllister et al., 2004). Individuals may frequently demonstrate cognitive deficits such as diminished memory for spatial information, decreased divided attention skills, working memory deficits, and impairments in general attention, problem-solving, and memory skills (Childers & Hux, 2016). Prevalence estimates of memory impairment in TBI range between 54 and 84%. Memory impairment can negatively impact and reduce the quality of life, and memory impairment varies across individuals with similar injury severity. Recent evidence suggests that working memory capacity may be one mediating variable that can help explain why cognitive reserve protects against long-term memory impairment (Sandry et al., 2014).
| Types of Traumatic Brain Injuries | |
|---|---|
| Concussion/Mild TBI | Loss of consciousness for up to 30 minutes; or confused or disoriented state lasting less than 24 hours; or memory loss lasting less than 24 hours. Excludes penetrating TBI. Results of a computed tomography (CT) scan, if obtained, are normal. |
| Moderate TBI | Loss of consciousness for more than 30 minutes, but less than 24 hours; or confused or disoriented state lasting more than 24 hours; or memory loss lasting more than 24 hours but less than 7 days; or meets criteria for concussion/mild TBI but with an abnormal CT. Excludes penetrating TBI. A structural brain imaging study may be normal or abnormal. |
| Severe TBI | Loss of consciousness for more than 24 hours; or confused or disoriented state lasting more than 24 hours; or memory loss lasting more than 7 days. Excludes penetrating TBI. A structural brain imaging study may be normal but usually is abnormal. |
| Penetrating TBI | Open head injury; scalp, skull, and dura mater (outer layer of meninges) are penetrated. Caused by high-velocity projectiles, objects of lower velocity such as knives, or bone fragments from a skull fracture that are driven into the brain. |

Introduction to Podcast

This podcast series’ primary focus is to spread awareness about TBI. Throughout these episodes, individuals will share their own experiences and stories. Professionals, caregivers, and TBI survivors share their insights and bring to light living with and caring for a TBI.
Listen Here: Introduction Podcast
Related External Links & Resources - General TBI Resources
- Quick Guide to Traumatic Brain Injury
- Mild Traumatic Brain Injury and Concussion:Information for Adults
- University Hospitals: Basic Information About Traumatic Brain Injury
- Brain Injury Recovery Step-by-Step
- Recovering from Mild Traumatic Brain Injury/Concussion: Summary Fact Sheet
- TBI Prevention, Rehabilitation, and Community Living: Health Brochure
- TBI Recovery and Prevention Resources
- Acquired Brain Injury and Family Violence
- Mild Traumatic Brain Injury/Concussion: Your Guide to Recovery
- CDC - Traumatic Brain Injury: In The United States - Emergency Department Visits, Hospitalizations and Deaths 2002–2006
- TBI: Prevention is the Only Cure
I have a TBI

TBI Survivor - Tatiana Gerowitz
Tatiana is a practicing artist and aspiring mathematics teacher. She resides in Davis, California and attends California State University, Sacramento. She suffered a TBI in 2017 after an automobile accident.
Listen Here: Tatiana's Podcast Interview

TBI Survivor - Eric Williams
Eric is a full-time fire prevention officer. He is a father and resides in Folsom, California. He suffered a TBI in 2015 after a running and bicycle accident.
Listen Here: Eric's Podcast Interview
Related External Links & Resources - TBI Survivor Resources
- Traumatic Brain Injury: A Guide For Patients
- A Guide for Patients and Families From Hospital to Home
- Traumatic Brain Injury Self-Advocacy: Advocating for Your Rights
- California Resources for Brain Injury Survivors
- Head Trauma Support Project of Sacramento
- Where to Start if Insurance Has Denied Your Service and Will Not Pay
- Brain Injury Support Groups in California
- Employee Rights in the Workplace
- College Guide for Students with Disabilities
- Parenting for Adults with Traumatic Brain Injury
Support Group Resources
- A Guide to Northern California Resources for Individuals with Brain Injury
- Brain Injury Association: Virtual Support Groups
- Del Oro Resource Center: Support Groups - Sacramento County
- Toolkit for TBI Support Group Facilitators
I Am Caring for Someone with a TBI

Mother of a TBI Survivor - Donna Long
Donna is a mother of three children and resides in the Sacramento area. She has been the primary caretaker of her son who suffered a TBI in 2019. She has been an advocate for her son and is motivated to share her experience to increase TBI awareness.
Caregiver and Family Resources
- BIUSA: Challenges, Changes, and Choices: A Brain Injury Guide for Families and Caregivers
- Mayo Clinic: Understanding Brain Injury - A Guide for the Family
- Mayo Clinic: Understanding Brain Injury - A Guide for the Family
- Ottawa Hospital: Brain Injury Caregiver - A Guide for Caregivers and Family
- Headway: The Family Guide to Brain Injury
- CDC: Help Your Child Be Successful at School After A TBI
- Family Guide to The Rancho Levels of Cognitive Functioning
- Headway: Caring for Someone with a Brain Injury
- Traumatic Brain Injury: Information for Parents
- TBI Bridge: Weekly Virtual Support Group Meeting for survivors, caregivers, family, and friends
Financial and Medical Insurance Resources
- BIAUSA: Adults & Brain Injury - Financial Issues
- Navigating the Insurance Maze after Brain Injury: A GUIDE FOR PATIENTS AND THEIR ADVOCATES
- BIAUSA: Is financial assistance available to people with brain injury and their families?
I Am Working with Someone who has a TBI

Speech-Language Pathologist - Elisabeth (Lisa) D'Angelo, M.S. CCC-SLP CBIS
Dr. Lisa D’Angelo has been a speech-language pathologist for 33 years in hospitals, rehabilitation centers, schools, early intervention, and university clinics. She received her bachelor’s degree in speech and hearing sciences from the UC, Santa Barbara, her master’s in communication disorders and sciences from San Jose State University, and her doctorate from UC Davis in human development (Language and Cognition). She is an associate professor at CSU, Sacramento, specializing in neurological development and disorders. Her research focus is on cognitive communication after traumatic brain injury (TBI) and dysphagia across the lifespan. She also works in the hospital setting, and as a school dysphagia/feeding specialist. She has presented locally, nationally, and internationally, and published articles about TBI, pediatric TBI, multi-disciplinary collaboration, and dysphagia, with a book chapter on cognitive-communication deficits in concussion/mild TBI.

Speech-Language Pathologist - Denise Kendrix, M.A. CCC-SLP
Denise graduated from the University of Redlands with a Bachelor of Arts degree in Communication Disorders and earned her Master of Arts degree in Speech Language Pathology from San Jose State University. She has worked in the medical setting for over 20 years with adults with cognitive, communication and swallowing disorders. She has a primary focus in traumatic brain injury and stroke and assists with facilitating the UC Davis Traumatic Brain Injury Support Group. She also is a volunteer board member for the Medical Speech Council of California.
Listen Here: Denise's Podcast Interview

Speech-Language Pathologist - Shannon Gassuan, M.S. CCC-SLP CBIS (Veteran Affairs)
Shannon is the Section Chief Speech-Language Pathologist at Sacramento VA Medical Center in Mather, California. She has been practicing in the field for over 20 years and works with TBI and other neurologic disorders. She is a part of the TBI Polytrauma team at Mather VA treating retired and active-duty military personnel with combat-related injuries.
Veteran's Resources
- Resources for Caregivers of Veterans with Traumatic Brain Injury
- Military Health System: A Guide for Caregivers of Service Members and Veterans
- I’m Caring for a Veteran with a Traumatic Brain Injury (TBI)- What do I need to know?
- Brainline: A Guide for Caregivers of Service Members and Veterans
- U.S. Department of Veterans Affairs: Polytrauma/TBI System of Care
- Clinician’s Guide to Cognitive Rehabilitation in Mild Traumatic Brain Injury: Application for Military Service Members and Veterans
- VA Polytrauma System of Care: Helping Veterans Get Back to Living
- Polytrauma Rehabilitation Family Education Manual
- Fact Sheet for Polytrauma and Traumatic Brain Injury
- California Veterans Handbook (p. 104)

Physiatrist - Dr. Topher Stephenson M.D.
Dr. Topher Stephenson, M.D. graduated from the University of New Mexico School of Medicine completed his residency in Physical Medicine & Rehabilitation at the University of California, Davis. Dr. Stephenson is board certified in both Physical Medicine & Rehabilitation and Brain Injury Medicine.
Listen Here: Dr. Stephenson's Podcast Interview

Physical Therapist - Dr. Katie Shinoda, DPT
Dr. Shinoda is a physical therapist at Mercy Outpatient Rehabilitation Center in Citrus Heights, California. She has been a practicing physical therapist for over 20 years and works with TBI and other neurologic disorders. She has worked in various stages of rehabilitation and recovery, including acute care, intensive care unit, and outpatient services. She currently practices physical therapy with individuals diagnosed with TBI and vertigo. She also organizes a grant-funded program for additional services for people with TBI trying to reintegrate into society.
Listen Here: Dr. Shinoda's Podcast Interview

Registered Nurse - Alyssa Francis, RN-BSN
Alyssa is a registered nurse at UC Davis Medical Center in Sacramento, California. She works in the medical surgery unit trauma patients including TBI. She is passionate about caring for and educating patients and their families.
Listen Here: Alyssa's Podcast Interview
Professional Resources:
- Mild Traumatic Brain Injury Rehabilitation Toolkit
- Traumatic Brain Injury: A Guidebook for Educators
- Barrow Neurological Institute & Dignity Health: Traumatic Brain Injury Patient and Family Handbook
- Mild Traumatic Brain Injury – Concussion: Pocket Guide for Clinicians
- Mayo Clinic: Understanding Brain Injury - A Guide for Employers
- Best Practices in The Management of Traumatic Brain Injury
- Clinical Practice Guidelines: Physical Therapy Evaluation and Treatment After Concussion/Mild Traumatic Brain Injury
- Traumatic Brain Injury Recovery Guide: Speech-Language Pathology
- Strategies Nurses Use When Caring for Patients With Moderate‐To‐Severe Traumatic Brain Injury Who Have Cognitive Impairments
- Guidebook for Psychologists: Working with Clients with Traumatic Brain Injury
Books & Literature
- "You Look Great!" -- Strategies for Living Inside a Brain Injury by John C. Byler, Laura Ricard
- Turn the Lights On!: A Physician’s Personal Journey from the Darkness of Traumatic Brain Injury (TBI) to Hope, Healing, and Recovery
- Our Daddy is Invincible by Shannon Maxwell
- Stroke Recovery Activity Book - Puzzles Workbook for Traumatic Brain Injury & Aphasia Rehabilitation
- Understanding Traumatic Brain Injury: A Guide for Survivors and Families
- Honey, I Smell Flowers: by Ruth Ann Bartels
- To Root & To Rise: Accepting Brain Injury
- I Am the Central Park Jogger: A Story of Hope and Possibility
- Over My Head: A Doctor's Own Story of Head Injury from the Inside Looking Out
- The Brain's Way of Healing: Remarkable Discoveries and Recoveries from the Frontiers of Neuroplasticity